SINGAPORE – It is now possible to walk into the newly opened Healthy Longevity Clinic at Alexandra Hospital (AH) as a “young senior” in one’s 50s or early 60s, go through a customised longevity programme and emerge with a “younger” body.
Launched on Thursday, the clinic is billed as the first in the world to open in a public hospital. It specialises in applying evidence-based medical treatments integrating geroscience and other disciplines of medicine to optimise health throughout one’s lifespan.
Geroscience, a field of research that studies the biology of ageing, has seen an acceleration in research over the last two decades, according to the United States Library of Medicine, the world’s largest medical repository.
What was once the preserve of the rich and famous who could afford to throw money at private longevity clinics is now available to the public in Singapore at, the clinic says, a fraction of the cost.
A baseline assessment and customised year-long care plan at the more than 50 sq m facility at AH costs upwards of $1,500, about a tenth of what it would cost at top private longevity clinics worldwide. The clinic is designed to be scalable to accommodate more than 3,000 individuals.
Dr Laureen Wang helms the clinic with a multidisciplinary team of specialists that includes longevity physicians, nurses, medical technologists, a health coach, a dietitian and an exercise physiologist.
She adds that the idea of longevity medicine is still new here and the individuals that the clinic sees are early adopters. They are referred to as individuals, not “patients” or “outpatients”.
“Singapore’s younger generation below the age of 35 are less concerned about health and ageing, and it is often only during times such as trying to conceive or when approaching midlife that they realise their bodies have changed,” says Dr Wang, 35, a practising cardiologist with AH and National University Health System (NUHS).
Pointing to the spartan backdrop of the clinic with its utilitarian furnishings, unlike posh private set-ups with cove lighting and designer lounge sets, she says: “We may not be located in a glamorous setting as there are less frills in a public hospital, but our longevity medicine teams will draw up a longevity road map to help individuals learn how to invest in health long after visiting the clinic, so he or she will be able to continue doing things at age 80 or 90, such as carrying grandchildren or walking up the stairs, which are a big boost for the quality of life.”
Healthspan versus lifespan
The focus of the clinic is on increasing healthspans through a holistic, evidence-based programme designed for Singapore’s rapidly ageing population that includes biomarker testing, lifestyle and dietary modifications, exercise and nutrition.
Unlike lifespan, which refers to the number of years from birth to death, healthspan is measured by the number of years a person remains in good health without a chronic or debilitating disease, well into the senior years from age 65.
The last nine to 10 years of a senior’s life are usually burdened by disease and poor quality of life, according to a 2021 report by the Regenerative Medicine journal, a London-based global peer-reviewed publication widely referred to by clinicians and policymakers.
It says that while lifespans were an important metric of health and well-being in the past, healthspans are now increasingly being measured because they show that it is not only important to live long, but also to be healthy and disease-free, thanks to recent strides in geroscience and longevity medicine.
Remote video URL
Healthspan is determined by one’s biological age, or the real age of the body, which may not be in sync with one’s chronological age. For instance, someone aged 50 may have a far lower biological age of 40, or a person aged 60 may be lumbering around with the body of a 75-year-old.
The higher the biological age, the higher the risk of chronic, age-related diseases.
Initiatives to help Singaporeans age well and remain in gainful employment longer were key highlights of Prime Minister Lee Hsien Loong’s National Day Rally speech on Aug 20, when he announced financial help for the retirement needs of lower- and middle-income Singaporeans aged 50 and above, whom he termed “young seniors”.
More seniors are also looking to stay economically active as long as possible as Singapore’s life expectancy at birth now ranks among the highest in the world.
According to the Department of Statistics, it was 64.5 years in 1965 and rose to 78 in 2000. Since 2022, Singaporeans can expect to live up to 83 years on average.
By 2030, one in four citizens here will be aged 65 and above. Singapore became an “aged” society in 2017, according to the United Nations, and will attain “super-aged” status by 2026.
How it works
Keeping costs low while making medical advances in geroscience available to the larger population is a priority for the team at AH’s Healthy Longevity Clinic.
To get a consult, there is no need for a doctor’s referral as the clinic is designed to be a walk-in medical centre. The public just needs to call for an appointment or send an e-mail (details below).
The diagnostic clinic works closely with the Centre for Healthy Longevity (Singapore), NUHS’ research facility co-located in AH, to come up with a customised programme that improves the rate of biological ageing for individuals aged 35 to 70. This includes young seniors, who are generally healthy or have at most one chronic disease such as diabetes or hypertension.
The individual’s biological age is determined through a battery of clinical tests that includes monitoring cardiovascular fitness, cognition, lung function and oral health, as well as blood work to assess metabolic, immune, liver, kidney and other organ functions.
Genes from one’s parents is believed to contribute to about 20 per cent of a person’s lifespan. Other factors that impact longevity include self-care, exercise, nutrition, sleep and exposure to the environment such as weather, pollution and noise.
Life expectancy of Singapore population rose in last decade but fell during Covid-19
World’s first clinic that aims to slow down ageing set to open in Singapore
Costs are determined after the physician has spoken to the individual to draw up a suitable care programme that is financially affordable and sustainable, time-wise.
The baseline assessment is not done to detect diseases, but to determine the individual’s state of health.
If a chronic disease shows up during the initial assessment, the individual may continue to be managed by the same team which follows AH’s model of integrated care to reduce further referrals. The individual may also be transferred to a relevant specialist in the chronic disease programme within the same hospital, if necessary.
As far as possible, the clinic relies on AH’s existing infrastructure and resources, such as laboratory, imaging and medical specialists.
Dr Grace Chiang, a consultant in family medicine who is one of the clinicians on the team, says individuals who are not aware that they have multiple comorbidities will not be turned away after signing up for the longevity programme.
“The management and focus of the longevity medicine may change as we continue to develop this service,” says Dr Chiang, 34.
“Rather than following the standard clinical programme, we may have to focus first on managing the individual’s chronic diseases,” she adds. “It depends on the type of chronic disease and the severity. Often, managing these chronic diseases takes priority as there can be an acceleration in biological ageing. Once the diseases are stabilised, we can discuss again about other interventions concerning healthspan.”
Another member of the team, Ms Cheryl Tan, 28, a health coach with AH, reviews each individual’s health status and works with the rest of the team to develop a health plan tailored to the individual’s needs and goals.
“With regular health coaching sessions, we will build on behavioural change to inculcate healthy habits in line with our treatment plan, which includes a combination of lifestyle interventions, such as dietary, exercise and sleep modifications, on top of medical interventions, such as medicines and supplements as recommended by the physicians,” she says.
Through providing ongoing support and motivation, Ms Tan encourages individuals to take ownership of their health and wellness to “live not just longer, but healthier”.
What it costs
A baseline assessment typically costs between $1,500 and $3,000 on a case-by-case basis, and includes a customised care programme that lasts about a year. This usually includes biomarker testing to determine the state of health at the outset, regular monitoring, and lifestyle modification consults on exercise and dietary changes.
In the United States, top private longevity clinics charge about US$100,000 (S$135,000) for customised care designed to keep affluent seniors in peak condition, according to a Wall Street Journal report in July.
Two private longevity clinics in Singapore are Chi Longevity at Camden Medical Centre and Regenosis at Ngee Ann City, both in the Orchard area. Chi was founded in March by leading global longevity expert Andrea Maier, who is also a director at the Centre for Healthy Longevity research centre in AH.
Professor Maier also provides guidance and recommendations to the clinic at AH regarding the structure of the service, suitability of diagnostics and interventions, and education and upskilling of health professionals to practise in the service. Her private clinic at Chi charges $15,000 for a customised plan and a 10-month journey to optimise health.
Prof Maier says Singapore is the only country she knows of that has established a longevity ecosystem bringing together pre-clinical and clinical research, clinical practice and public health.
“No other country is at the forefront of optimising the health of all citizens,” she adds.
Regenosis was founded in 2019 by former real estate developer Shaun Lim, 55. The clinic charges from $500 for in-house customised packages to about $31,000 for stem cell treatments.
Dr Wang says there are plans to make the practice of longevity medicine more affordable and accessible to a greater segment of the population so that Healthy Longevity Clinics proliferate throughout Singapore. This will help to bring costs down further with more tie-ups with a range of specialities currently available in other hospitals.
There is currently no government subsidy available at her Alexandra Hospital clinic.
“One of our goals on a national level is to demonstrate cost effectiveness of the care we provide and eventually work with the Ministry of Health and policymakers to enable this service to be subsidised for Singaporeans,” she adds.
Info: Call the NUHS Contact Centre on 6908-2222 or e-mail the Healthy Longevity Clinic at AH_Wellness@nuhs.edu.sg, giving your full name and contact number for an appointment. For updates, go to www.ah.com.sg
Good mental health can improve longevity: Local study
Body balance training for longevity and quality of life
Cutting-edge tools to determine ‘real’ age
The Healthy Longevity Clinic at Alexandra Hospital leverages breakthroughs from the National University Health System’s research facility Centre for Healthy Longevity (Singapore) to offer a comprehensive approach to health and longevity.
It starts with a baseline assessment using a range of tests, from blood biomarkers for cardiovascular risk factors to tests measuring an individual’s exercise capacity. It also deploys advanced techniques such as epigenetics and artificial intelligence (AI) to determine an individual’s biological or “real” age.
Here are some of the tools it uses:
1. Advanced Glycation End-products (AGEs) Reader
The AGEs Reader is a non-invasive device that uses ultraviolet (UV) light to detect autofluorescence in human skin tissue, which, in layman terms, refers to the interaction of light with molecules in the skin such as proteins, lipids and collagen.
By measuring the level of AGEs in skin tissue, it is possible for clinicians to estimate an individual’s biological age. AGEs are formed when sugar molecules react with proteins and lipids in the body. They are associated with a number of chronic diseases including diabetes, cardiovascular disease and kidney disease.
There is a 12-second exposure to UV rays on the arm during this procedure, which is less exposure than standing outdoors under the sun for a few minutes.
The AGEs Reader is not a diagnostic test as it is used primarily to assess the risk of developing chronic diseases.
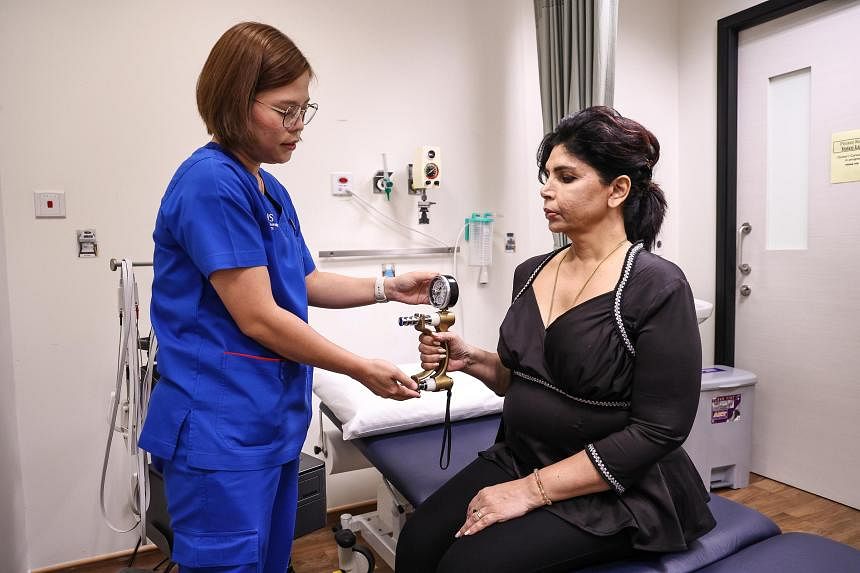
2. Dynamometer Handgrip Strength
This test is a simple and quick way to measure muscle strength in the hands and forearms. It is a reliable test that can be used to assess physical function and identify those at risk of frailty and falls.
It is performed using a dynamometer, a hand-held device that measures the amount of force one can apply with the grip. The individual sits with an arm bent at a 90-degree angle while holding the device handle and squeezing with all of his or her might.
While the normal range for handgrip strength varies depending on age, gender and body size, in general, a handgrip strength of less than 18kg for women and less than 28kg for men is considered to be on the lower end.
Low handgrip strength can be a sign of frailty, a condition characterised by a decline in physical function and an increased risk of falls and other health problems.
Frailty is a major public health problem, estimated to affect more than 20 per cent of adults over the age of 65.
3. Pulse Wave Velocity
This is a quick and painless tool to measure the age of the blood vessels through arterial stiffness.
The individual lies on an examination bed for 15 minutes. A cuff is first placed around the arm to measure blood pressure and, after that, on the thigh.
The distance from the neck to the thigh is measured to give the clinician an idea of how fast the pulse travels in the major blood vessels, which is related to how stiff the vessels are.
A probe is then gently placed on the neck to detect the pulse.
The stiffer the arteries, the faster the pulse wave travels.
Arterial stiffness is associated with a number of cardiovascular risk factors such as age, hypertension, diabetes and smoking.
4. Bioelectrical Impedance Assessment (BIA)
Also known as bioelectrical impedance spectroscopy, this is a non-invasive test that measures the resistance of the individual’s body to a small electrical current. The resistance is affected by the amount of water and fat in the body.
The BIA estimates body composition including body fat percentage, muscle mass, skeletal muscle mass and the hydration status of an individual to monitor changes in body composition over time.
It is a quick and painless test that takes just two minutes and is performed while the individual sits on a bed or chair. Three pairs of electrodes are placed on the ankles, the thumbs and middle fingers. A small electrical current is then passed through the body.
The resistance of the body to the current is then measured and used to calculate the total body composition. The BIA gives the doctor information about the individual’s tissue anatomy and physiology which can indicate degeneration or accelerated ageing.
5. Bone Mineral Density
The full body scan provides an analysis of body composition – bone as well as soft tissues. It is a fundamental part of a nutritional status assessment, and the use of diagnostic imaging methods helps clinicians determine lean body mass as well as fat mass.
This whole-body densitometry scan, which takes 15 minutes, uses dual-energy X-ray absorptiometry, also called Dexa.
The scan can also be used to diagnose osteoporosis, monitor its progression and assess responses by the individual to interventions.
6. Electrocardiogram (ECG) Monitoring Patch
Lightweight and portable ECG heart rate monitoring devices are used in the clinic to assess heart rate patterns and palpitations. These may come in a wearable wrist strap or as an adhesive patch attached to the chest.
The patch is to be worn for 24 hours after leaving the clinic, then returned a day later. The lightweight, shower-proof patch allows the individual the freedom to get on with daily routines while wearing it.
Such devices are used to assess a range of heart conditions such as abnormal heart rhythms (arrhythmia) or, as in this case, to aid in exercise prescription.
Taking a peek inside my 64-year-old body
When I volunteered for a battery of tests at the Healthy Longevity Clinic at Alexandra Hospital for this feature, I knew exactly what I was signing up for. Or thought I did.
There was overwhelming trepidation at what the results would reveal. My mind kept coming up with hyperboles. Would the clinicians detect abnormalities? Would they cart me off in a stretcher for immediate admission?
Fortunately, it was a very calming experience as the genial specialists the six testing stations seemed to know exactly what to say.
“How are you feeling, Ms Chantal? I hope you’re okay?”
That was a good opener. No one addressed me as “madam”. And there was none of that gendered ageism or “lookism” (judging people according to their looks) at this clinic.
I went through five tests to give clinicians an instant readout of my overall health and posed for one test (full body scan) for illustrative purposes only, as the results would take a little longer to compute.
The full body scan has been a hit on social media, with American celebrities such as Kim Kardashian, Paris Hilton and Cindy Crawford posting about how it helped them gain peace of mind through a range of imaging scans to detect the early onset of diseases such as breast cancer.
I donned a robe and lay down without a pillow under my head for about 15 minutes to simulate a session on the Dexa, which is a dual-energy X-ray absorptiometry scan that uses low-dose X-rays for bone density and body fat composition analysis.
Mr Lim Seong Yong, senior radiographer at AH’s Diagnostic Imaging Centre, patiently posed for photographs as my imagination ran riot over what the scan would pick up.
Would it show a porous skeleton with degenerative bone disease? Or would it pick out dark masses usually associated with The Big C?
Hardly the stuff that would compel me to pose like Kardashian on Instagram in August, where she shared about her low body fat percentage and strong bones.
I lay there in my vulnerability, resisting the urge to get up and run. All for you, dear reader.
I had to omit some biomarker assessments such as blood age (determined through a standard panel of blood tests and then calculated using AI algorithms), as the results would arrive long after this article is published. Some of these tests are sent to AH laboratories and others to external labs in Singapore and other countries. Results usually take two to four weeks to come back.
The first test I did was the Dynamometer Handgrip Strength test, in which I squeezed a metal device that was monitored by senior staff nurse Er Biaw Thean.
For my vintage, Ms Er remarked that the reading is usually less than 30kg. But she pointed out that I had notched 34kg, and asked the director of the clinic, Dr Laureen Wang, to analyse the results after more tests.
I then went through the Pulse Wave Velocity assessment to find out the age of my blood vessels, through taking blood pressure readings from my right arm, left thigh and neck. This was to measure how fast the pulse travels in the major blood vessels, which is related to how stiff the vessels are.
After that, it was the Bioelectrical Impedance Assessment (BIA), where electrodes were strapped to my ankles, middle fingers and thumbs.
These tests, which showed a combination of negative and positive readouts, needed to be combined with the full suite of assessments to give doctors a more accurate picture of my health.
There were some triumphs for not-so-humble brags.
“The handgrip reading, together with your BIA results, shows that you have been exercising regularly to maintain your muscle mass in your core and limbs,” observed Dr Wang. “In fact, your muscle mass is better than expected compared with peers in your age group.”
Score!
She advised me to continue with my daily yoga routine, good for both muscle and bone health, as well as eat more fish such as salmon, and kale and spinach, which furnish calcium and vitamin D.
I left the room beaming and brimming with third-quarter resolutions to up my dose on the right foods and do more Surya Namaskar (Sun Worship) deep yoga stretches.
Then I was bundled into more rooms for more tests to piece together a pastiche of my biological age.
The next stop was the Advanced Glycation End-products Reader, which determines skin autofluorescence through sugar molecules. I inserted my left forearm into the machine, which looked like a desktop printer with a slot, where a beam of ultraviolet light passed through my forearm.
This test gives doctors an idea of chronic conditions such as diabetes and cardiovascular disease. The results showed that I was in the “red zone”, meaning I had a high percentage of sugar molecules, though I do not suffer from diabetes or hypertension.
As I began to worry, health coach Cheryl Tan cautioned it was just a preliminary scan and that it would be taken again after lifestyle modifications and more testing. Some comfort, but okay, I filed it away as work in progress, to be continued.
The last test involved an exercise and shower-proof wearable device for monitoring heart functions, which was glued to my chest for 24 hours, starting from that afternoon – a Monday. The duration varies according to the individual being treated.
The readings were interpreted by Dr Wang two days later.
Living to be 100: Call for society, govts to start planning
Teach seniors right to reap ‘longevity dividend’ from Singapore’s ageing population: Panel
Generally (and thankfully), my heart rate range was good. Dr Wang detected a low asymptomatic heart rate in the early morning which she declared all right for a “fit individual” like myself.
Wow. My heart leapt at “fit” – definitely a Kardashian moment.
“The heart rate variability over 24 hours is good,” Dr Wang went on. “Studies have shown individuals with lower heart rate variability are in poorer health and have suboptimal coping mechanisms for emotional or physical stressors, and a higher risk of mortality.”
Some of the cutting-edge assessment tools and technology such as blood age, determined through blood samples, are not commonly available in Singapore clinics. I made a mental note to free my schedule to sit through the complete range of biomarker assessments at a later date.
After all, my motto towards ageing is very simple: Fight it or die trying. My goal is the biological age of a 28-year-old, which best reflects how I feel inside.
Clarification note: An earlier version of this article stated that the longevity clinic can help people have a body 10 years younger. The clinic has clarified that the figure was derived from previous research.
Join ST’s Telegram channel and get the latest breaking news delivered to you.
p.st_telegram_boilerplate:before {
display: inline-block;
content: ” “;
border-radius: 6px;
height: 6px;
width: 6px;
background-color: #12239a;
margin-left: 0px;
margin-right: 13px;
}
a.st_boilerplate {
font-family: “SelaneWebSTForty”, Georgia, “Times New Roman”, Times, serif;
}